Ringworm in Cats: Percy’s Case
 My cat Percy turned 16 this March. For almost his entire life, he was a healthy, hardy, active cat; but everything changed in the spring of 2007. That spring was the start of a series of bacterial and fungal infections that led me to my topic: Ringworm in cats. Ringworm is a skin disease caused by any of a handful of different fungi that grow on the surface of the skin, causing irritation. To fully explain my cat’s case, I have to start with a previous infection.
My cat Percy turned 16 this March. For almost his entire life, he was a healthy, hardy, active cat; but everything changed in the spring of 2007. That spring was the start of a series of bacterial and fungal infections that led me to my topic: Ringworm in cats. Ringworm is a skin disease caused by any of a handful of different fungi that grow on the surface of the skin, causing irritation. To fully explain my cat’s case, I have to start with a previous infection.
During spring break of my sophomore year at Cornell, I came home and noticed that one of Percy’s toes on his left front foot was hairless and swollen. My mom took him to the vet, who explained that it was most likely just irritation that would go away. When I came home from school in May, it had not gotten any better; in fact, Percy’s entire left front foot was hairless and very pink. We took him back to the vet, and this time he performed a culture that came back with positive results for a notorious bacterium: MRSA, methicillin-resistant Staphylococcus aureus. Percy was instantly put on antibiotics, which he took until the spring of 2008. At that point, Percy’s hair was growing back and we performed another culture that confirmed he was no longer infected…all-clear, right? Wrong.
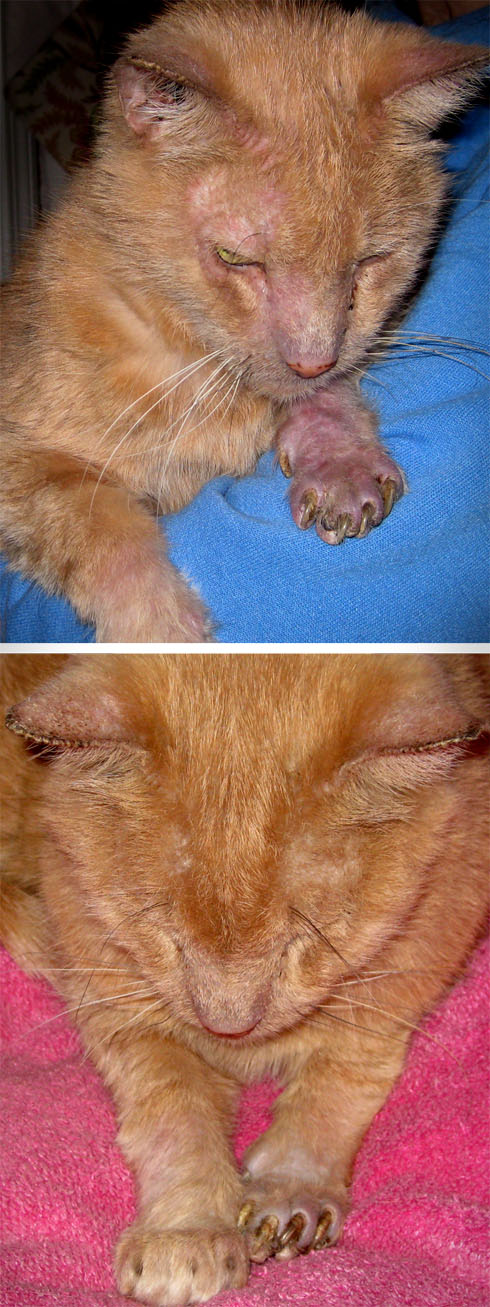 The following summer, Percy started losing fur again, except this time it spread about a third of the way up his left front leg and onto his face and right front leg. We took him to the vet frequently but were at a loss as to what could be causing it. Percy was also scratching his head a lot. The vet was scratching his head too, and said it probably wasn’t a fungus like ringworm because cats don’t normally get those infections unless they have depressed immune systems. By fall, we still didn’t know what was wrong with our cat even after taking him to another veterinarian, but my family was experiencing fungal infections of our own. Each member of my immediate family was treated for ringworm, and I had an infection on my elbow that a nurse at Cornell’s Gannett Health Services said was the “biggest she had ever seen.” Ringworm in people can be acquired from animals, and a cluster of cases in a family implicates a common source like the family pet. So when I was home for fall break, my mother and I took Percy to the second vet again and asked if, against all odds, it could actually be ringworm. He didn’t think so, because it didn’t present normally–no red, raised, or circular lesions, and when he looked at Percy’s face under a Wood’s lamp it did not fluoresce.** However, the vet pulled some hairs from Percy’s face and sent them to a laboratory who would see if anything could be grown from them.
The following summer, Percy started losing fur again, except this time it spread about a third of the way up his left front leg and onto his face and right front leg. We took him to the vet frequently but were at a loss as to what could be causing it. Percy was also scratching his head a lot. The vet was scratching his head too, and said it probably wasn’t a fungus like ringworm because cats don’t normally get those infections unless they have depressed immune systems. By fall, we still didn’t know what was wrong with our cat even after taking him to another veterinarian, but my family was experiencing fungal infections of our own. Each member of my immediate family was treated for ringworm, and I had an infection on my elbow that a nurse at Cornell’s Gannett Health Services said was the “biggest she had ever seen.” Ringworm in people can be acquired from animals, and a cluster of cases in a family implicates a common source like the family pet. So when I was home for fall break, my mother and I took Percy to the second vet again and asked if, against all odds, it could actually be ringworm. He didn’t think so, because it didn’t present normally–no red, raised, or circular lesions, and when he looked at Percy’s face under a Wood’s lamp it did not fluoresce.** However, the vet pulled some hairs from Percy’s face and sent them to a laboratory who would see if anything could be grown from them.
About a week later, we received a call from the vet, who told us Percy did indeed have ringworm, and that the fungus Microsporum canis was the culprit. He also recommended we run tests for feline AIDS (FIV) and feline leukemia virus (FeLV) to see if one was the underlying cause of immune depression leading to Percy’s fungal infection. The tests came back positive for FIV, and in the meantime Percy started treatment with itraconazole, an antifungal drug. The vet wasn’t optimistic about Percy’s chances of recovery, but after a few months of oral medicine and medicated Sebolux baths Percy started to regrow hair, stopped itching, and his skin looked much less dry. We thought, once again, that we were out of the tunnel.
We thought too soon. In spring, Percy started losing fur again, this time worse than before. We kept shampooing him but it wasn’t helping, so we brought him back to the vet. This time, the culture revealed a different agent of ringworm–a species of the fungus Trichophyton. Percy’s prescription was changed to oral fluconazole, a different antifungal drug, and within about 6 months Percy’s hair had grown back again. One final culture came back negative for the various fungi that cause ringworm, so Percy was finally free of his infections.
The second vet we took Percy to was fascinated by his case. He talked to veterinary dermatologist colleagues about it, to get their opinions and compare notes. Ringworm is common in shelter cats, as the causative fungi can spread very easily among cats,4 but it is less common for an individual cat in a house to become infected. As I said before, cats have natural immunity when they are healthy, but kittens less than one year of age1 and immune-depressed cats are at risk. Cats self-clean, and this practice may remove fungal spores, assisting in immunity to fungal infections.6 Ringworm is three times more likely to occur in FIV-positive cats, who are more susceptible to a number of diseases. A cell-mediated response is necessary for recovery from ringworm,5 but FIV affects the T-cells of the cat’s immune system,3 allowing FIV-positive cats to become easily infected and making recovery very hard. Vaccines have been produced for cattle and there is a commercial vaccine for cats as well, but its availability is limited5 and more research is needed.2 Another interesting fact that my family experienced is that cats are the main source of human infections1 and that at least one person in 70% of households with an infected cat will experience ringworm infections of their own.5
While Percy was at risk for ringworm because of his FIV, thankfully he has now recovered from his infections. He may never fully regrow hair on his ears (they’re covered with peach fuzz now) and he won’t be winning any beauty contests, but at least he is relatively healthy again. I wanted to share this experience and some of the knowledge I have gained as a result.
**Editor’s Note: An ultraviolet Wood’s Lamp is often used to support diagnosis of ringworm (dermatophyte) infection. Some of the various ringworm infections in animals will fluoresce under a Wood’s Lamp. But not all: Individual strains of Microsporum canis may or may not fluoresce.
Works Cited:
- Cecchi, S, Corazza, M, Mancianti, F, Nardoni, S, and Taccini, F. Dermatophytes isolated from symptomatic dogs and cats in Tuscany, Italy during a 15-year-period. Mycopathologia 156 (2002): 13-18.
- DeBoer, D.J, and Lund, A. Immunoprophylaxis of Dermatophytosis in Animals. Mycopathologia 166 (2008): 407-424.
- Feline Immunodeficiency Virus. Cornell University College of Veterinary Medicine. Cornell Feline Health Center. 15 November 2006.
- Hodge, Kathie. Dermatophytes I. Cornell University PLPA 3290 lecture, 4 February 2010.
- Newman, C. Facts about Ringworm. Newman Veterinary Medical Services. 2010.
- Ringworm In Cats – General Overview Of The Disease. Ringworm in Cats. Ringwormincats.org. 2010.


Over a period of several years, I experienced numerous ringworm infections, some quite serious, covering up to 90% of my body. Eventually, I realized that each and every case of ringworm had occurred after I was exposed to pyrethrins – both the natural kinds and the synthetic spinoffs. My most recent case occurred after I started taking feverfew for cluster headaches. I try to avoid all pesticides now.
Wow Damon, that sounds harrowing. So pyrethrin exposure seems to make you more susceptible to ringworm? I’ve not heard this before, and I’m no expert on pyrethrins. Skin irritation resulting from pyrethrin exposure could possibly make it easier for the dermatophytes to become established.
My feline has a similar condition called eosinophilic granuloma complex, after intense research and grilling the veterinarian about all the possible anecdotes – we went with an immunosuppressive therapy and systemic glucocorticoids. Not fun!